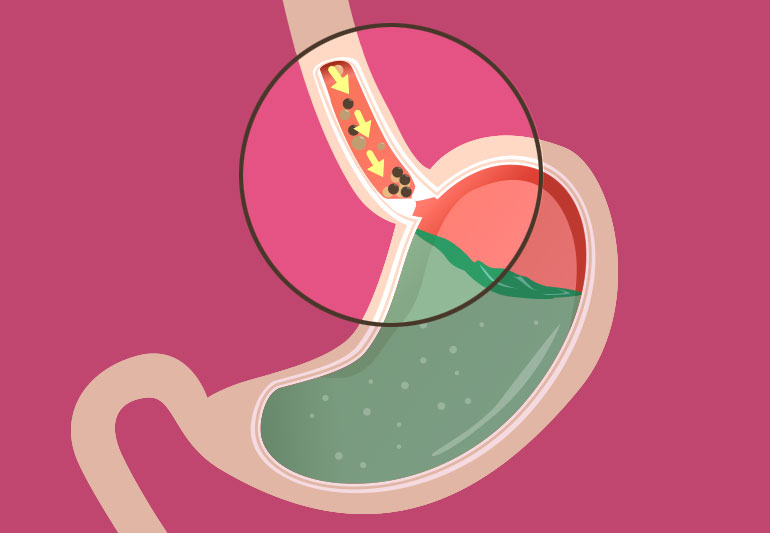
Achalasia of oesophagus is a condition where the lower oesophageal sphincter (LES) is dysfunctional leading to altered motility of the oesophagus. The LES becomes very tight, not allowing solid food to pass down easily into the stomach. The causes of LES dysfunction are unknown, and caused can be due to nerve degeneration due to autoimmune and infectious causes. This leads to patients unable to eat and drink normally leading to weight loss and malnourishment. Patients also present with recurrent vomiting, and bad breadth due to food stasis in the oesophagus. Many a time, the patient will be unaware of the symptoms, and can the symptoms can also be similar to cancer of the distal oesophagus.
Classical history of swallowing difficulties, recurrent vomiting and younger age points towards achalasia. The following investigations help in establishing the diagnosis:
A tiny video camera attached to a slender, flexible tube is passed down into the stomach through the throat and the esophagus. The endoscope transmits images of the stomach on to a television screen for the doctor to see. The LES area is closely examined to ensure no cancerous lesion exists, and if anything suspicious, then the endoscopist will take a specimen for biopsy. Endoscopy will also reveal dilated esophagus and tight LES, indicating achalasia.
This is the next test usually recommended. In this test, a small tube is placed in the esophagus via the nose for 24 hours, and is attached to a recorder which is kept with the patient. This test will show the resting pressure of LES (usually high in achalasia) and also the motility pattern of the esophagus which helps in classifying achalasia into 3 types.
Endoscopy and Manometry tests will be sufficient to clinch the diagnosis. Other tests like barium swallow and CT scan will be recommended deepening on the type and extent of achalasia.
20 + years of Experience
500+ Surgeries
1000+ Happy patients
75+ Esphageal cancer treated
The treatment recommendation is based on patient’s health and severity of achalasia. The following treatments are recommended:
Once the diagnosis of achalasia is confirmed, the doctor will put down an endoscope through the mouth to the site of LES. A balloon is then placed across the sphincter, and gradually dilated with saline to a certain pressure enough to disrupt the muscle fibres of the LES. It offers temporary relief, and may need repeated attempts to give symptomatic relief. It is not a permanent solution, and the patient will end up needing a POEM or laparoscopic surgery to address it.
In POEM, the surgeon carries out the procedure via the endoscope introduced through the mouth. Using specialised instruments, the surgeon makes a small cut on the inner lining of the esophagus and creates a tunnel under the mucosal layer all the way up to the tight lower esophageal sphincter. The LES is then divided using a small knife via the endoscope, and the mucosal incision in the esophagus higher above is closed with clips. The patient has a check endoscopy and dye swallowing test the following day to confirm no side effects from the procedure. The patient is discharged after 1 day and can resume normal diet. Currently, POEM has equivalent results to laparoscopic surgery, and remains scarless. There is a slightly higher risk of reflux, and the advice would be appropriately given.
This has been the ‘ gold standard of treatment’ for many years with good outcomes and resolution of symptoms. This procedure is done laparoscopically/ key hole method which gives quicker recovery. Small cuts are made on the abdomen, and surgeon uses laparoscopic instruments to perform the surgery. The surgeon makes a cut over the LES sphincter area to divide the muscle fibres only (protecting the inner lining mucosa) and follows the cut with a fundoplication procedure ( stomach wrap) to prevent acid reflux from stomach into oesophagus. The surgery usually lasts 2-3 hours and most patients are discharged within 1-2 days.
Post achalasia surgery ( endoscopy or surgery), the patient will require dedicated endoscopic screening every 2-3 years depending on the severity pre-procedure. Due to increased acid reflux post treatment, the patient’s are prone to develop changes in the lining in the lower esophagus leading to esophagitis, BARRETT’S esophagus and in small proportion of patients, development of cancer. Hence, endoscopic screening is the only method to keep an eye out for these developments.
WhatsApp us